Tail-Cuff Blood Pressure in Mice and Rats: Do It Right So Your Data Hold Up
TL;DR Tail-cuff blood pressure can be fast, scalable, and reliable—when you treat it like physiology instead of a device demo. Most bad runs come from the same few issues: stress, poor tail perfusion, movement, and inconsistent session design. This guide explains what tail-cuff is actually measuring, why acclimation and warming matter, how awake and anesthetized workflows differ, and how to troubleshoot failure modes without “re-running until something looks nice.”
Tail-cuff Blood Pressure is a solid method—and it’s sensitive to the variables that move blood pressure.
Tail-cuff blood pressure is one of the most practical ways to measure BP in mice and rats without surgically implanting devices. It scales well, it can be repeatable, and it’s widely used for screening and cohort studies.
The limitation isn’t the method. It’s the measurement site.
Tail-cuff systems detect changes in tail blood volume and flow while the cuff cycles. Tail perfusion responds quickly to temperature, stress, and movement—the same variables that influence blood pressure in vivo. When any of these shift during a session, you can see failed cycles, increased variability, or results that don’t align with prior runs.
The good news is that these problems are usually predictable and fixable.
This article explains what tail-cuff blood pressure is measuring, how to stabilize perfusion with acclimation and temperature control, what changes in awake vs anesthetized workflows, and how to troubleshoot the most common failure modes without turning data collection into trial-and-error.
What tail-cuff blood pressure is really measuring
Tail-cuff systems don’t measure blood pressure “at the heart.” They detect changes in tail blood volume/flow while the cuff occludes and releases. That’s why the same animal can produce beautiful cycles one day and garbage the next: the tail is the measurement site, and tail blood flow is sensitive to stress and temperature.
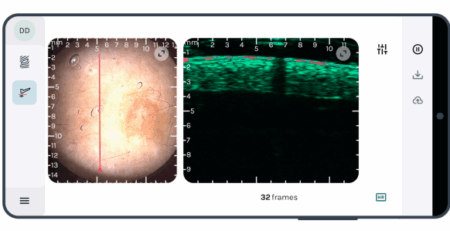
With Volume Pressure Recording (VPR), the system tracks tail blood volume changes using a sensor during cuff cycling. The practical advantage is simple: you can tell whether you’re getting a usable physiological signal or just squeezing a tail and hoping for meaning. In VPR-based systems, diastolic can be measured rather than inferred, which can matter depending on your endpoints and how tightly you need to characterize pressure dynamics.
The big implication: if tail perfusion is poor, nothing downstream is going to save you—not software settings, not more cycles, not wishful thinking.
Acclimation is not a nice-to-have. It’s the data.
If you’re measuring awake animals, acclimation is where your “non-invasive blood pressure monitor” becomes a real tool instead of a coin flip.
Acclimation isn’t about being gentle. It’s about reducing the stress response and movement that distort readings. A mouse that’s fighting restraint is giving you “BP under stress + motion artifacts,” even if you label the column “baseline.”
A good acclimation approach is boring and consistent. Short sessions, repeated exposure to the holder, consistent timing, and a stable environment. You’re teaching the animal that the holder and cuff aren’t a crisis. When that clicks, your signal quality improves and your cycle success rate stops being a gamble.
If you want your readings to represent physiology rather than panic, this is where you earn it.
Warming isn’t just comfort. It’s signal quality.
Tail perfusion is a bottleneck;literally. If blood vessels in the tail aren’t dilated enough, you won’t see signal, period. Warming is one of the most effective ways to improve it—especially in mice, cold rooms, or sessions where handling has reduced peripheral flow.
But warming needs to be consistent. “Sometimes we warm, sometimes we don’t, sometimes the pad is set differently” is a recipe for variability that looks like biology. It isn’t.
The goal is simple: establish repeatable conditions where the tail has stable blood flow across animals and across days. That’s why a controlled warming approach matters. If you’re building a dependable station, RightTemp® and RightTemp® Jr. are designed for exactly this kind of repeatability.
Over-warming isn’t clever either. Too much heat can change physiology, increase agitation, and make your “fix” the new confound. You’re aiming for stable perfusion—not a sauna.
Awake vs anesthetized: pick the trade-off you can defend
Both approaches can be valid. The key is understanding what changes so you’re not surprised by “better signal” that’s actually altered physiology.
Awake measurements: closer to baseline, harder to execute
Awake tail-cuff blood pressure measurements can be the better choice when BP is a primary endpoint and you don’t want anesthesia influencing cardiovascular physiology. The cost is that you now have to manage stress and motion as experimental variables. That’s doable, but it requires acclimation discipline and consistent operator technique.
If your awake runs are unstable, the fix is rarely “more cycles.” It’s usually improving acclimation, stabilizing perfusion, and tightening the session design so you’re not measuring during the worst part of the animal’s stress curve.
Anesthetized measurements: cleaner signal, different physiology
Anesthesia typically reduces motion artifacts, which can make the signal look cleaner. The trade-off is that anesthetic depth, protocol, and downstream temperature drift can significantly influence BP and heart rate during the run. If you go this route, temperature control is not optional. It stops blood vessels from constricting, creating the difference between a stable physiologic window and a slow drift that makes your session inconsistent at best, and not work at all at worst
If anesthetized runs are part of your workflow—especially paired with imaging environments— the CODA is built for those conditions
Your holder setup matters
Restraint is the uncomfortable truth of non-invasive tail BP: you need stability to measure, but restraint itself can create the stress response you’re trying to avoid.
The win is not “tight restraint.” The win is stable positioning with minimal struggle and unobstructed breathing. When the animal is positioned consistently and can settle, motion artifacts drop and cycle validity improves.
CODA’s nose cone holders are designed around that practical reality—visibility, breathing, and consistent positioning for tail-cuff blood pressure work.
The failure modes you might see, and how to fix them without guessing
“It keeps failing cycles”
When cycles fail repeatedly, the most common culprit is poor tail perfusion (or a leaky cuff, but that’s easy to fix). Before you chase software settings, stabilize the basics: consistent warming, stabilization time after placement, correct cuff sizing, and a calmer animal (which loops you back to acclimation).
A lot of people try to brute-force their way out of this by running longer. That usually makes it worse, because you’re extending the time the animal is stressed and moving.
“Numbers jump all over the place”
Wild variability across cycles is typically motion + stress. You can’t average your way out of panic. You need the animal to settle and the environment to stop changing.
This is where session structure matters: a defined stabilization window, a defined number of cycles, and a consistent rule for discarding obvious artifacts. Not “throw out the bad ones until the mean looks nice,” a real rule you’d be comfortable describing to someone reading your methods.
“Values drift during the session”
Drift often comes from temperature drift (especially anesthetized), slow acclimation settling (awake), or simply making the session too long.
The fix is usually tightening the session and controlling what’s drifting. If temperature is moving, you can’t pretend the BP you measured at minute 2 is comparable to minute 18. Control temperature and keep the measurement window consistent.
“Works in rats, falls apart in mice”
Mice are less forgiving. Small changes in perfusion, stress, cuff placement, and ambient temperature have bigger effects. If your rat workflow “kind of works,” your mouse workflow will expose every weak link.
For mice, treat acclimation and warming as first-class requirements, not optional extras. Use a setup you can run the same way every time.
A session structure that stays honest
You don’t need a complicated protocol, but you do need one you can repeat.
A solid session has three characteristics:
- the animal is given time to acclimate to the holder (or anesthesia)
- perfusion conditions are consistent
- you run a defined number of cycles and report results with a consistent artifact rule
When you do that, tail-cuff blood pressure stops feeling like a magic trick and starts behaving like a measurement tool.
If you’re building a station that can scale from “a few animals” to multiple cohorts, the hardware and software workflow matters. CODA was designed for that: CODA® Monitor and CODA® High Throughput System.
Choosing a Tail-cuff blood pressure solution
If you want a sanity check on your setup—awake vs anesthetized, acclimation plan, warming approach, cohort size—contact a specialist to get your workflow recommendation today.